Intra-abdominal adhesions in ultrasound. Part II: The morphology of changes
Andrzej Smereczyński1, Teresa Starzyńska1, Katarzyna Kołaczyk2, Stefania Bojko3, Maria Gałdyńska3, Elżbieta Bernatowicz3, Anna Walecka2
 Affiliation and address for correspondence
Affiliation and address for correspondence
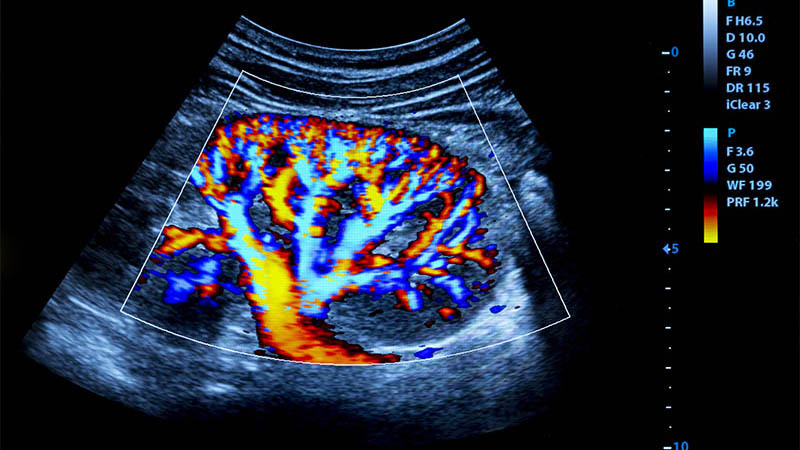
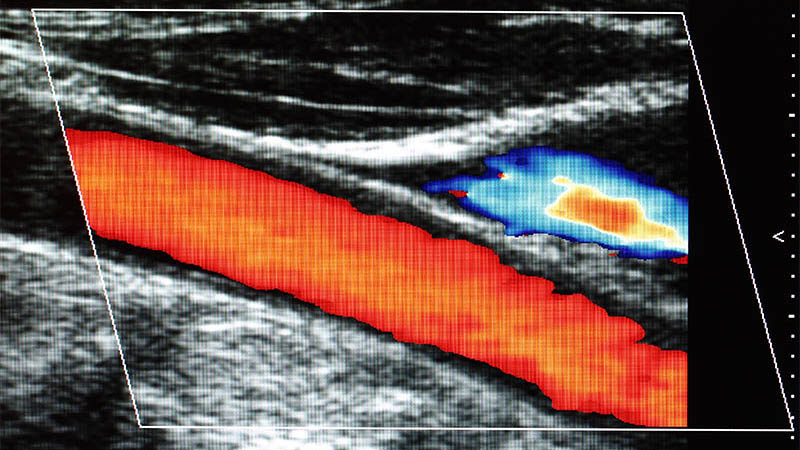
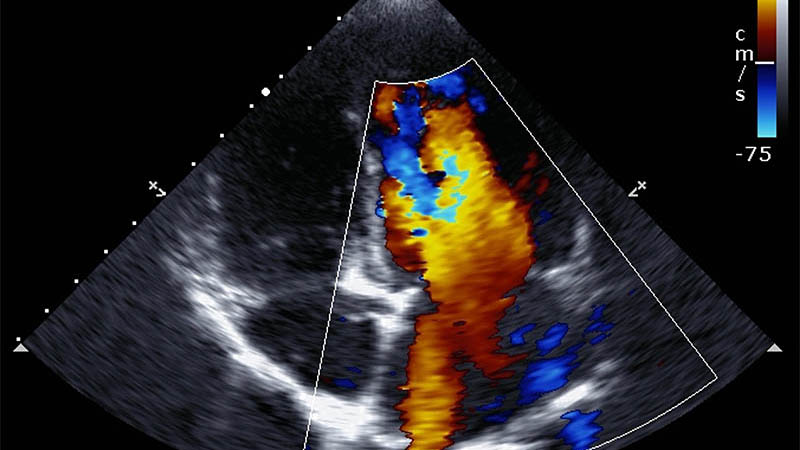
Despite their frequent appearance, intra-abdominal adhesions are rarely the subject of clinical studies and academic discussions. For many years the operators have been trying to reduce such unfavourable consequences of interventions in the abdominal structures. The aim of this article is to present the possibilities of intra-abdominal adhesion diagnostics by means of ultrasound imaging based on authors’ own experience and information included in pertinent literature. The anatomy and examination technique of the abdominal wall were discussed in Part I of the article. In order to evaluate intraperitoneal adhesions, one should use a convex transducer with the frequency of 3.5–6 MHz. The article provides numerous examples of US images presenting intra-abdominal adhesions, particularly those which appeared after surgical procedures. The significance of determining their localisation and extensiveness prior to a planned surgical treatment is emphasized. Four types of morphological changes in the ultrasound caused by intra-abdominal adhesions are distinguished and described: visceroperitoneal adhesions, intraperitoneal adhesions, adhesive obstructions as well as adhesions between the liver and abdominal wall with a special form of such changes, i.e. hepatic pseudotumour. Its ultrasound features are as follows:
1. The lesion is localised below the scar in the abdominal wall after their incision.
2. The lesion is localised in the abdominal part of the liver segments III, IV and V.
3. With the US beam focus precisely set, the lack of fascia – peritoneum complex may be noticed. An uneven liver outline or its ventral displacement appears.
4. A hepatic adhesion-related pseudotumour usually has indistinct margins, especially the posterior one, and, gradually, from top to bottom, loses its hypoechogenic nature.
5. In a respiration test, this liver fragment does not present the sliding movement – a neoplastic tumour rarely shows such an effect. The immobility of the liver is a permanent symptom of subdiaphragmatic abscess which needs to be included in the differentiation process.
6. In case of doubts, the suspicious liver area may be examined without the consideration of the scar in the abdominal wall.
In the differentiation of visceroperitoneal adhesions, firstly, one needs to exclude the peritoneum infiltration in the course of inflammation and neoplastic spreading, which may be very difficult in patients who have undergone a surgery. Pseudomyxoma peritonei constitutes a source of errors much more rarely.